Demand for insurance claims fraud detection solutions is growing; new report outlines market sizing and vendors serving this space
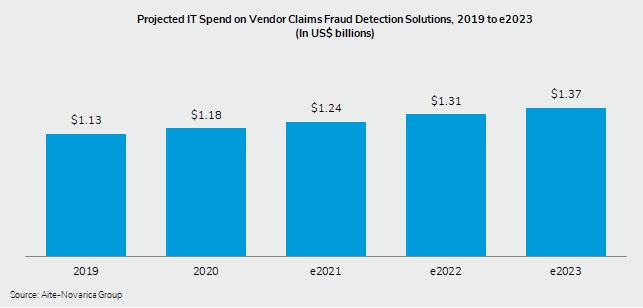
As technological advancements have made crimes such as identity theft and claims manipulation easier to commit and harder to detect, digitalization is creating a variety of new data sources that insurers can use to identify fraudulent behavior. In a new Impact Report, Market Overview: P/C Claims Fraud Detection Solutions, research and advisory firm Aite-Novarica Group examines the state of the claims fraud detection solution market and lists key market trends affecting fraud detection specific to P/C claims as well as the vendors serving this space.
“Initiatives to enhance customer experience and improve operational efficiency, such as claims automation, have only amplified fraud risk,” said Stuart Rose, Strategic Advisor at Aite-Novarica Group. “Insurers are implementing real-time fraud detection techniques to detect and prevent opportunistic and organized fraud across multiple lines of business and jurisdictions.”
“Some fraud detections solutions are better for certain lines of business,” adds Martina Conlon, Head of Property/Casualty Insurance at Aite-Novarica Group and co-author of the new report. “Geography, market, and claims types all affect fraud detection models. It’s critical to ensure that vendor strengths align with insurer business objectives.”
A preview of the report is available online, and desk copies are available to qualified media. Please contact [email protected] or call Kaitlyn Labbe at +1.857.327.9442 for more information.
About Aite-Novarica Group:
Aite-Novarica Group is an advisory firm providing mission-critical insights on technology, regulations, strategy, and operations to hundreds of banks, insurers, payments providers, and investment firms—as well as the technology and service providers that support them. Comprising former senior technology, strategy, and operations executives as well as experienced researchers and consultants, our experts provide actionable advice to our client base, leveraging deep insights developed via our extensive network of clients and other industry contacts. Visit us on the web and connect with us on Twitter and LinkedIn.
Press Contact:
Kaitlyn Labbe
Public Relations
+1.857.327.9442
[email protected]
