February 9, 2023 – Establishing and maintaining satisfaction with providers in the health plan network is perhaps a payer organization’s most critical operational goal. Strategies for enhancing provider satisfaction are straightforward but not always easy to implement, and healthcare payer organizations’ track record is surprisingly inconsistent. This inconsistency is an opportunity for attentive organizations to position themselves as industry leaders, while laggards may be signing up for headaches and thorny provider relationships.
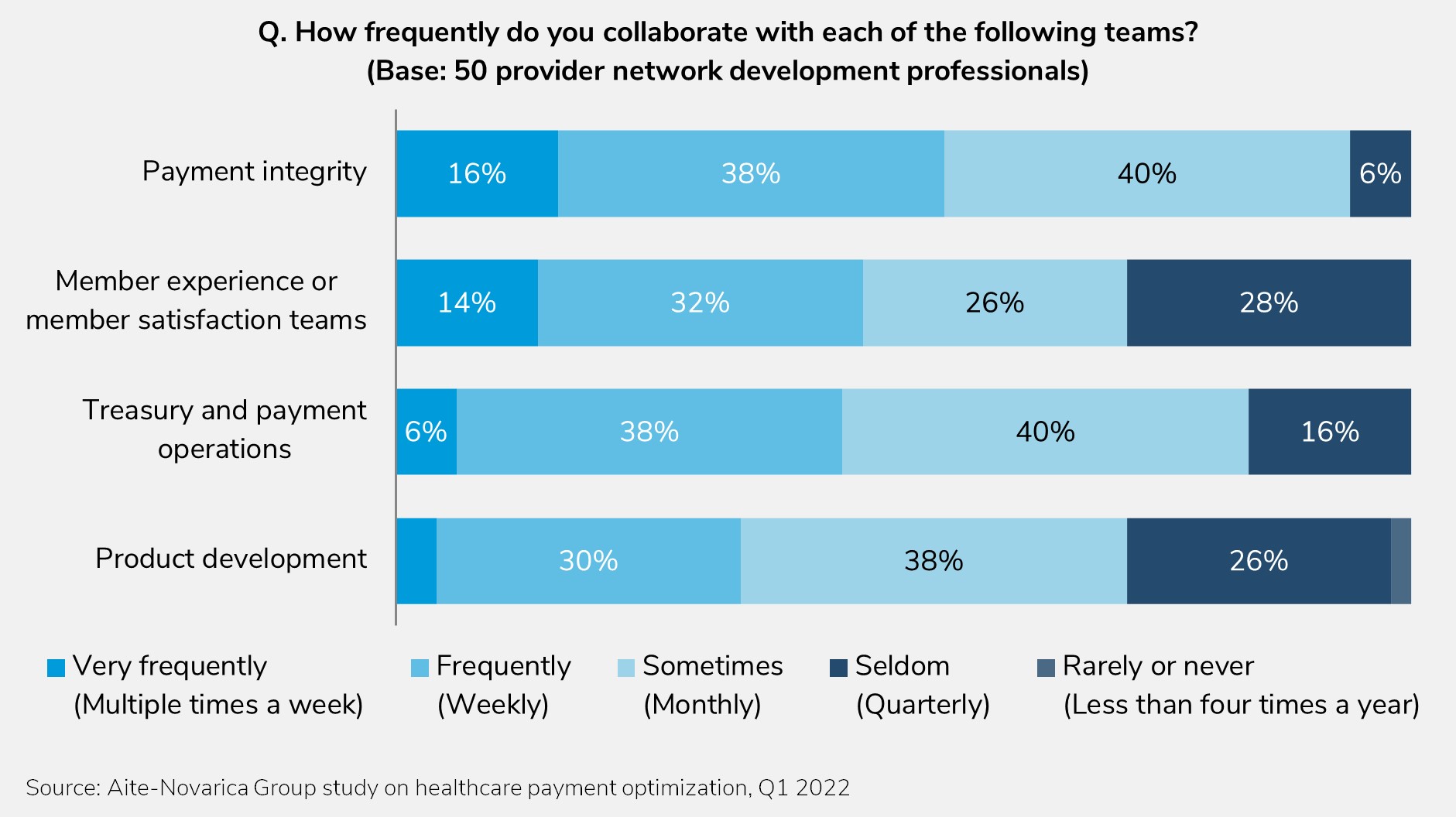
This report offers an outline for the next generation of payer-provider relationships to enhance engagement via technology and automation. This study is based on an Aite-Novarica Group Q1 2022 survey of 214 healthcare payer executives.
Clients of Aite-Novarica Group’s Healthcare Payments service can download this report and the corresponding charts.
About the Author

Erika Baumann
Erika Baumann serves as Director of the Commercial Banking & Payments practice at Datos Insights, focusing on payables and receivables technology and solutions. She has over 10 years of experience in the wholesale banking space, bringing expertise from both banking and fintech vendor positions. She has worked extensively with both U.S. and international banks, vendors, and the clients of each to identify...
