February 2, 2023 – For health plans that grapple with cost containment and preserving their provider networks, increasing focus on provider satisfaction—both prior to claim submissions and after—can be a valuable differentiator. Increasing focus entails relationship building, aligned incentives, and agreement on a common set of operating metrics. While the personal touch that builds relationships cannot be automated, technology can nevertheless streamline some repetitive processes.
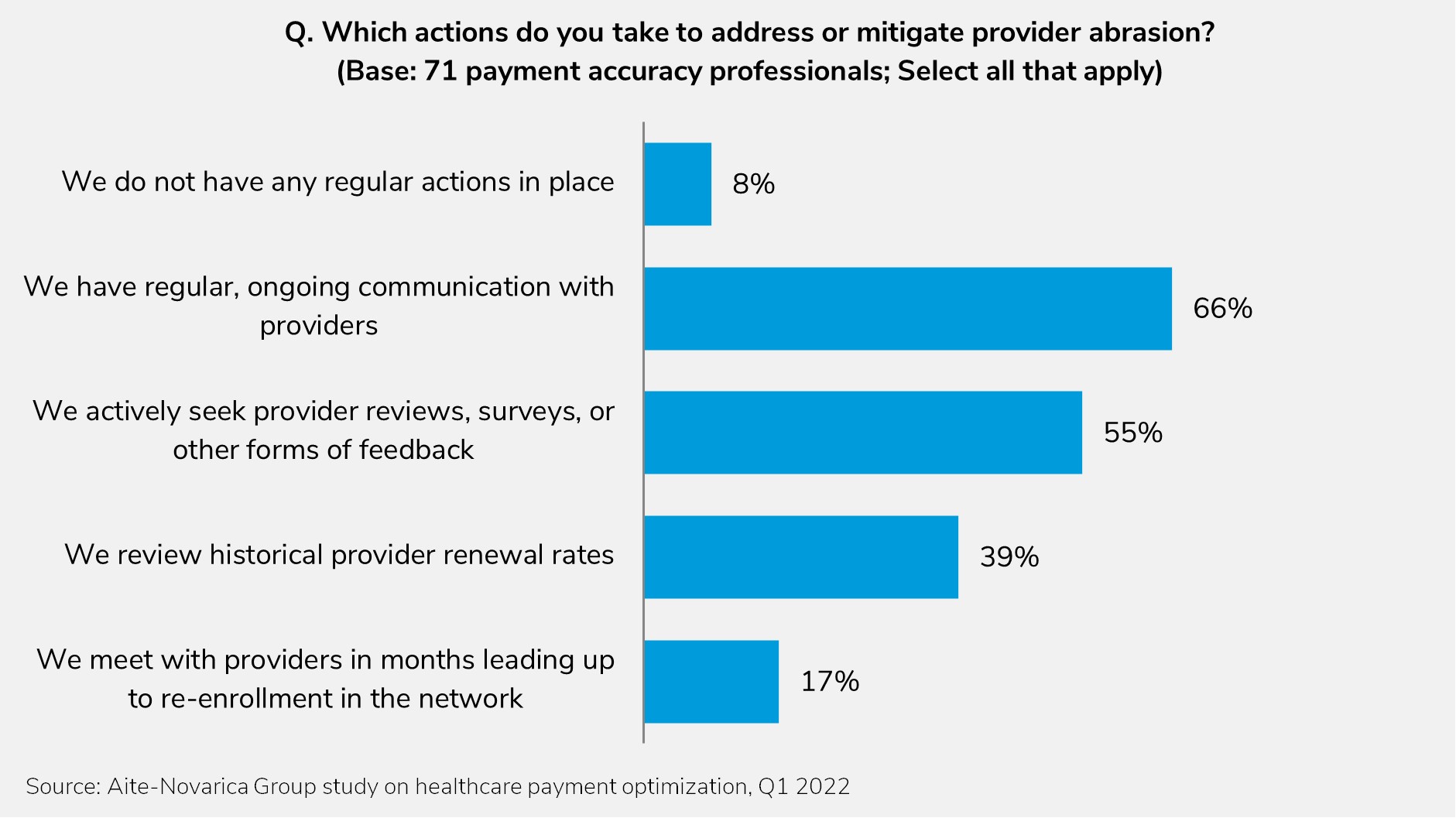
This report assesses how payment integrity and cost containment professionals across U.S. healthcare payers are applying data, analytics, and automation in their processes to address the biggest gaps and opportunities. This study is based on an Aite-Novarica Group Q1 2022 survey of 214 healthcare payer executives.
Clients of Aite-Novarica Group’s Healthcare Payments service can download this report and the corresponding charts.
About the Author

Erika Baumann
Erika Baumann serves as Director of the Commercial Banking & Payments practice at Datos Insights, focusing on payables and receivables technology and solutions. She has over 10 years of experience in the wholesale banking space, bringing expertise from both banking and fintech vendor positions. She has worked extensively with both U.S. and international banks, vendors, and the clients of each to identify...
