The forecast for 2023 will be a mix of changing dynamics, new headwinds, and an economic environment in flux.
- Shifting dynamics are taking automation and cloud deployments up in the form of technology innovations, as health firms embrace new automations to enhance payment capabilities and get comfortable with cloud architectures and embedded banking from financial services.
- Headwinds are sweeping through the healthcare environment, from smaller brokers and advisors brewing up competition against major health plans to expanded usage of Medicare Advantage plans and Affordable Care Act (ACA) exchanges.
- An economic environment in flux adds complexity with a mix of high interest rates, inflation, and tepid returns on market investments, but it has also opened the door to alternative benefits that may reshape the employer benefits landscape in the coming decade.
These factors do not present a “doom and gloom” situation for healthcare players, but instead they create new opportunities for growth and innovation. The challenge for health plans and payers in 2023 is to identify how digital payment methods, strategies, and services are expanded, both to withstand current pressures and emerge with improved operational efficiencies as an organization.
Aite-Novarica Group has distilled the developments in healthcare payments into 10 top trends that will influence the industry in 2023.
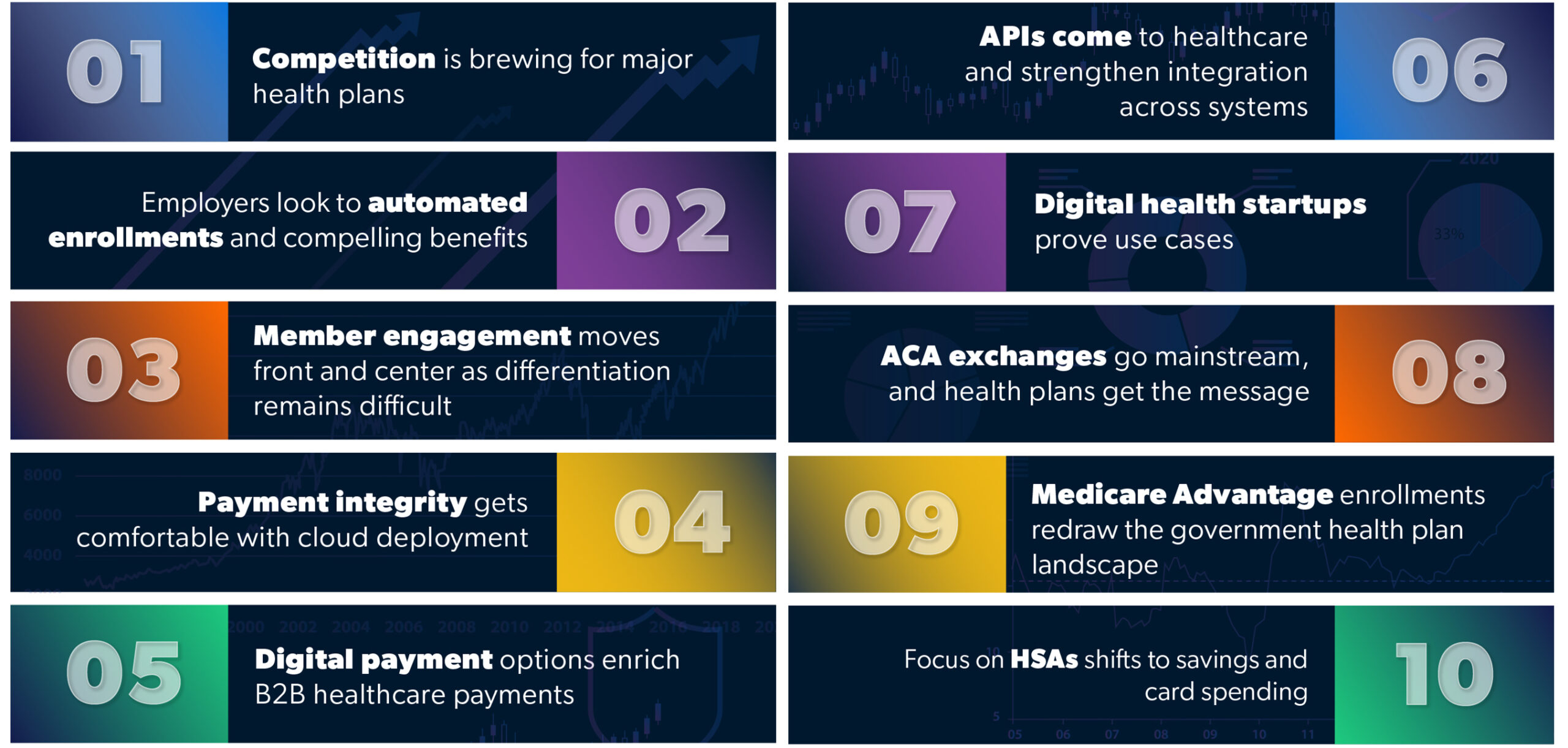
Some of these include:
- Growing interest in digital payment methods streamlines B2B payments: Healthcare payments are dominated by the “Big Three” of paper checks, wire transfers, and ACH transactions, but digital payment options are growing in relevance. Electronic check conversions, virtual cards, and peer-to-peer (P2P) networks like Zelle match, and in many cases exceed, the speed and data reconciliation of ACH payments. Additionally, real-time capabilities offer powerful use cases for healthcare, from automated reconciliations and account-to-account payments to real-time claims and explanation of benefits (EOB) access.
- APIs come to healthcare, making integration (and innovation) easier: APIs swept through financial services and are now making their mark in healthcare and health payments. APIs are bread and butter for cloud deployments, alleviating the financial resources otherwise dedicated to building and maintaining legacy middleware and software. APIs also inject flexibility and interoperability into the tech stack and open the gate for integration with vendors to enable automated payments and increased information exchange with other third-party applications. Ultimately, APIs will be the key to creating new products and services, including embedded banking and financial ones, that can be built on an intuitive, user-friendly portal.
- Brewing competition against health plans: While health plans had strong earnings in 2022, they should be mindful of competition and discontent in their membership base, competitors, and industry partners. While the following factors are not likely to shake health plans from their position of power in 2023, they do reflect important sentiments from health plan members. This may come in the form of narrower networks; incentives to nudge members to high-quality, lower cost providers in the form of steerage; or other creative approaches.
- Members continue to be discontent with high premiums and out-of-pocket costs. While lower utilization in 2020 and 2021 due to COVID-19 meant that medical loss ratios (MLRs) freed up some premium payments to be returned to plan members, concerns remain surrounding healthcare premiums.
- Competitors, particularly small and regional health plans, lament the challenge of competing with mega health plan structures now dominating the market after years of merger and acquisition activity.
- Industry partners, namely small- and medium-size third-party advisors and some benefits brokers such as those oriented to the Health Rosetta model, are changing course, promoting low- or no-deductible plans and direct primary care plans.
- Focus on Health Savings Accounts (HSA) shifts to savings and card spending: The Fed’s interest rate hikes will impact the bottom line of custodians and revenue share partners in a positive manner. Additionally, stagnation in the market and lukewarm investment sentiments will lead account holders with investments to search for alternatives when allocating their funds. Custodians, banks, and revenue share partners will consider promoting high-yield saving account options and determining how much of the interest rate increases to share with individual account holders. Emphasis on expanding the use of prepaid HSA/FSA cards will also increase.
Areas like member engagement, automated enrollments, and payment integrity are also set for changes, setting up 2023 as a challenging and transformative year.
To learn more about the top ten trends in healthcare that Aite-Novarica Group has identified for 2023, click here to download the full report and reach out at [email protected] to share what you think will impact your industry in 2023. You can also watch the recording of our February 16th webinar, where we explored each of these trends in detail. Click here to access the recording.